| General Discussion Undecided where to post - do it here. |
| Reply to Thread New Thread |
|
|
#1 |
|
|
Unfortunately, at the same time that Western mental-health professionals have been convincing the world to think and talk about mental illnesses in biomedical terms, we have been simultaneously losing the war against stigma at home and abroad. Studies of attitudes in the United States from 1950 to 1996 have shown that the perception of dangerousness surrounding people with schizophrenia has steadily increased over this time. Similarly, a study in Germany found that the public’s desire to maintain distance from those with a diagnosis of schizophrenia increased from 1990 to 2001.
Researchers hoping to learn what was causing this rise in stigma found the same surprising connection that Mehta discovered in her lab. It turns out that those who adopted biomedical/genetic beliefs about mental disorders were the same people who wanted less contact with the mentally ill and thought of them as more dangerous and unpredictable. This unfortunate relationship has popped up in numerous studies around the world. In a study conducted in Turkey, for example, those who labeled schizophrenic behavior as akil hastaligi (illness of the brain or reasoning abilities) were more inclined to assert that schizophrenics were aggressive and should not live freely in the community than those who saw the disorder as ruhsal hastagi (a disorder of the spiritual or inner self). Another study, which looked at populations in Germany, Russia and Mongolia, found that “irrespective of place . . . endorsing biological factors as the cause of schizophrenia was associated with a greater desire for social distance.” Even as we have congratulated ourselves for becoming more “benevolent and supportive” of the mentally ill, we have steadily backed away from the sufferers themselves. It appears, in short, that the impact of our worldwide antistigma campaign may have been the exact opposite of what we intended. NOWHERE ARE THE limitations of Western ideas and treatments more evident than in the case of schizophrenia. Researchers have long sought to understand what may be the most perplexing finding in the cross-cultural study of mental illness: people with schizophrenia in developing countries appear to fare better over time than those living in industrialized nations. This was the startling result of three large international studies carried out by the World Health Organization over the course of 30 years, starting in the early 1970s. The research showed that patients outside the United States and Europe had significantly lower relapse rates — as much as two-thirds lower in one follow-up study. These findings have been widely discussed and debated in part because of their obvious incongruity: the regions of the world with the most resources to devote to the illness — the best technology, the cutting-edge medicines and the best-financed academic and private-research institutions — had the most troubled and socially marginalized patients. Trying to unravel this mystery, the anthropologist Juli McGruder from the University of Puget Sound spent years in Zanzibar studying families of schizophrenics. Though the population is predominantly Muslim, Swahili spirit-possession beliefs are still prevalent in the archipelago and commonly evoked to explain the actions of anyone violating social norms — from a sister lashing out at her brother to someone beset by psychotic delusions. McGruder found that far from being stigmatizing, these beliefs served certain useful functions. The beliefs prescribed a variety of socially accepted interventions and ministrations that kept the ill person bound to the family and kinship group. “Muslim and Swahili spirits are not exorcised in the Christian sense of casting out demons,” McGruder determined. “Rather they are coaxed with food and goods, feted with song and dance. They are placated, settled, reduced in malfeasance.” McGruder saw this approach in many small acts of kindness. She watched family members use saffron paste to write phrases from the Koran on the rims of drinking bowls so the ill person could literally imbibe the holy words. The spirit-possession beliefs had other unexpected benefits. Critically, the story allowed the person with schizophrenia a cleaner bill of health when the illness went into remission. An ill individual enjoying a time of relative mental health could, at least temporarily, retake his or her responsibilities in the kinship group. Since the illness was seen as the work of outside forces, it was understood as an affliction for the sufferer but not as an identity. For McGruder, the point was not that these practices or beliefs were effective in curing schizophrenia. Rather, she said she believed that they indirectly helped control the course of the illness. Besides keeping the sick individual in the social group, the religious beliefs in Zanzibar also allowed for a type of calmness and acquiescence in the face of the illness that she had rarely witnessed in the West. The course of a metastasizing cancer is unlikely to be changed by how we talk about it. With schizophrenia, however, symptoms are inevitably entangled in a person’s complex interactions with those around him or her. In fact, researchers have long documented how certain emotional reactions from family members correlate with higher relapse rates for people who have a diagnosis of schizophrenia. Collectively referred to as “high expressed emotion,” these reactions include criticism, hostility and emotional overinvolvement (like overprotectiveness or constant intrusiveness in the patient’s life). In one study, 67 percent of white American families with a schizophrenic family member were rated as “high EE.” (Among British families, 48 percent were high EE; among Mexican families the figure was 41 percent and for Indian families 23 percent.) Does this high level of “expressed emotion” in the United States mean that we lack sympathy or the desire to care for our mentally ill? Quite the opposite. Relatives who were “high EE” were simply expressing a particularly American view of the self. They tended to believe that individuals are the captains of their own destiny and should be able to overcome their problems by force of personal will. Their critical comments to the mentally ill person didn’t mean that these family members were cruel or uncaring; they were simply applying the same assumptions about human nature that they applied to themselves. They were reflecting an “approach to the world that is active, resourceful and that emphasizes personal accountability,” Prof. Jill M. Hooley of Harvard University concluded. “Far from high criticism reflecting something negative about the family members of patients with schizophrenia, high criticism (and hence high EE) was associated with a characteristic that is widely regarded as positive.” Widely regarded as positive, that is, in the United States. Many traditional cultures regard the self in different terms — as inseparable from your role in your kinship group, intertwined with the story of your ancestry and permeable to the spirit world. What McGruder found in Zanzibar was that families often drew strength from this more connected and less isolating idea of human nature. Their ability to maintain a low level of expressed emotion relied on these beliefs. And that level of expressed emotion in turn may be key to improving the fortunes of the schizophrenia sufferer. Of course, to the extent that our modern psychopharmacological drugs can relieve suffering, they should not be denied to the rest of the world. The problem is that our biomedical advances are hard to separate from our particular cultural beliefs. It is difficult to distinguish, for example, the biomedical conception of schizophrenia — the idea that the disease exists within the biochemistry of the brain — from the more inchoate Western assumption that the self resides there as well. “Mental illness is feared and has such a stigma because it represents a reversal of what Western humans . . . have come to value as the essence of human nature,” McGruder concludes. “Because our culture so highly values . . . an illusion of self-control and control of circumstance, we become abject when contemplating mentation that seems more changeable, less restrained and less controllable, more open to outside influence, than we imagine our own to be.” CROSS-CULTURAL psychiatrists have pointed out that the mental-health ideas we export to the world are rarely unadulterated scientific facts and never culturally neutral. “Western mental-health discourse introduces core components of Western culture, including a theory of human nature, a definition of personhood, a sense of time and memory and a source of moral authority. None of this is universal,” Derek Summerfield of the Institute of Psychiatry in London observes. He has also written: “The problem is the overall thrust that comes from being at the heart of the one globalizing culture. It is as if one version of human nature is being presented as definitive, and one set of ideas about pain and suffering. . . . There is no one definitive psychology.” Behind the promotion of Western ideas of mental health and healing lie a variety of cultural assumptions about human nature. Westerners share, for instance, evolving beliefs about what type of life event is likely to make one psychologically traumatized, and we agree that venting emotions by talking is more healthy than stoic silence. We’ve come to agree that the human mind is rather fragile and that it is best to consider many emotional experiences and mental states as illnesses that require professional intervention. (The National Institute of Mental Health reports that a quarter of Americans have diagnosable mental illnesses each year.) The ideas we export often have at their heart a particularly American brand of hyperintrospection — a penchant for “psychologizing” daily existence. These ideas remain deeply influenced by the Cartesian split between the mind and the body, the Freudian duality between the conscious and unconscious, as well as the many self-help philosophies and schools of therapy that have encouraged Americans to separate the health of the individual from the health of the group. These Western ideas of the mind are proving as seductive to the rest of the world as fast food and rap music, and we are spreading them with speed and vigor. No one would suggest that we withhold our medical advances from other countries, but it’s perhaps past time to admit that even our most remarkable scientific leaps in understanding the brain haven’t yet created the sorts of cultural stories from which humans take comfort and meaning. When these scientific advances are translated into popular belief and cultural stories, they are often stripped of the complexity of the science and become comically insubstantial narratives. Take for instance this Web site text advertising the antidepressant Paxil: “Just as a cake recipe requires you to use flour, sugar and baking powder in the right amounts, your brain needs a fine chemical balance in order to perform at its best.” The Western mind, endlessly analyzed by generations of theorists and researchers, has now been reduced to a batter of chemicals we carry around in the mixing bowl of our skulls. All cultures struggle with intractable mental illnesses with varying degrees of compassion and cruelty, equanimity and fear. Looking at ourselves through the eyes of those living in places where madness and psychological trauma are still embedded in complex religious and cultural narratives, however, we get a glimpse of ourselves as an increasingly insecure and fearful people. Some philosophers and psychiatrists have suggested that we are investing our great wealth in researching and treating mental illness — medicalizing ever larger swaths of human experience — because we have rather suddenly lost older belief systems that once gave meaning and context to mental suffering. If our rising need for mental-health services does indeed spring from a breakdown of meaning, our insistence that the rest of the world think like us may be all the more problematic. Offering the latest Western mental-health theories, treatments and categories in an attempt to ameliorate the psychological stress sparked by modernization and globalization is not a solution; it may be part of the problem. When we undermine local conceptions of the self and modes of healing, we may be speeding along the disorienting changes that are at the very heart of much of the world’s mental distress. http://www.nytimes.com/2010/01/10/ma...pagewanted=all I thought this was interesting as I was always interested in those curious syndromes with varied but sometimes crippling symptoms usually lacking a clear pathology which seem to appear out of the blue and get a lot of media exposure for a while and then slowly fade away, as if losing popularity. It seems the expression of these 'diseases' must be crucially concerned with culture and obscure some underlying wrong, which is depression or anxiety related. I mean things like electromagnetic hypersensitivity, which would improbably qualifiy as a normal hypersensitivity (allergy) as there is no pathogen and double-blind tests consistently fail to find a correlation between EM fields and symptoms. When this was very much in the news a decade ago my mother was quite insistent that I don't spend to much time in the vicinity of computer screens, because apparently my skin would flush... http://en.wikipedia.org/wiki/Electro...persensitivity Other popular, but hard to define and pin down and therefore to treat, typically Western syndromes are fibromyalgia, Chronic Lyme disease and other heterogenic pain syndromes with unspecific (or unproven) pathology. The difficulty obviously being to distinguish them (I'm trying to avoid calling them hypochondrias) from more 'real' chronic pains, such as neuralgia, which can definitely be crippling. http://en.wikipedia.org/wiki/Fibromyalgia In India, a there's a syndrome called dhat, where the (presumably very anxious) male patients believe they are losing their semen in their urine and becoming impotent. And there are various others: http://en.wikipedia.org/wiki/Culture-bound_syndrome http://en.wikipedia.org/wiki/Dhat Another issue here is the reaction that schizophrenics get in our modern Western (perhaps Americanized) culture and whether that might in actuality be harmful. Do you know any schizophrenics? What was your and and other people's reaction when they found out? Thoughts? |
|
|
|
|
#2 |
|
|
|
|
|
|
|
#3 |
|
|
Oh sorry, I was led to believe that every post on this forum was a joke. I apologize.
I think that the attempts by the scientific elite, in this case psychologists, to characterize even the most mundane of human behaviors as "syndromes", "diseases", and the like is offensive, and should be regarded as nothing less than a direct challenge to the species and to human nature itself. Quite a bold challenge coming from a pseudo-science like psychology. |
|
|
|
|
#4 |
|
|
|
|
|
|
|
#5 |
|
|
Psychiatric treatments do not have a pleasant history. Especially recently, anti-depressants and the like have been found to do more harm than good. It was found from toxicological analyses that a lot less (n=420) of more than 17000 suicidal patients from 1995-2005 had traces of anti-depressants in their body compared to a control group (600). This would mean that 500-600 suicides are prevented each year in the national population, a huge amount. Edit: There were no pharma companies involved in this particular study. I'd have to read up on it to be able to speak more authoritatively, and I realize that studies from other parts of the world may not have found a similar protective effect, but to claim that psychiatry (or psychology - which is a different field!) are "most dangerous" seems hysterical. If you don't trust science about mental illness, who do you trust? By no means am I implying blind trust or that scientists are infallible or don't produce contradictory results at times, but trust in the scientific method and consensus over time. Edit, a relevant graph:  Anti-depressant use (in cyan) rising, while suicides (in lilac) drop. |
|
|
|
|
#6 |
|
|
I can't read Swedish, but that graph doesn't seem to correlate very well.
From Selective Serotonin Reuptake Inhibitor (SSRI) Drugs: More Risks Than Benefits?: "At most 30% of patients receive a benefit from SSRIs beyond the large placebo effect in certain mental conditions...Adverse effects are common, occurring in up to 75% of subjects. Severe adverse effects may be under reported." Anecdotal reports of severe problems for anti-depressant pateints are extensive in the U.S. I don't think characterizing the situation as most dangerous is hysterical when you have very young SSRI patients carrying out umpteen school shootings. In fact I'd like to see a graph with anti-depressant use and deaths via school shootings. Might leave a different impression than the one above. |
|
|
|
|
#8 |
|
|
|
|
|
|
|
#9 |
|
|
|
|
|
| Reply to Thread New Thread |
«
Previous Thread
|
Next Thread
»
| Currently Active Users Viewing This Thread: 1 (0 members and 1 guests) | |
|
|


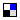


 Linear Mode
Linear Mode


